How to Identify Scabies: Signs and Visual Clues
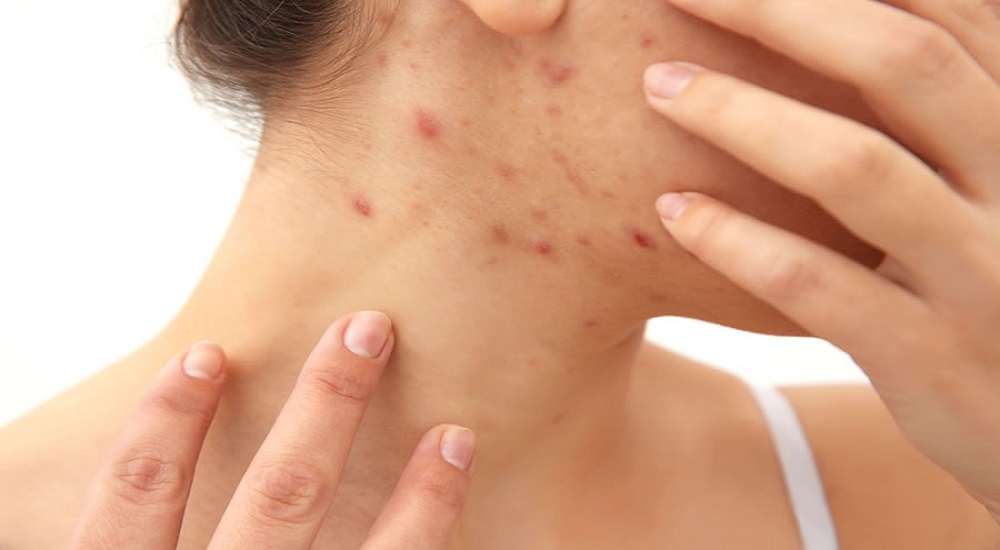
Scabies, often referred to as the “seven-year itch,” is an irritating and contagious skin condition caused by tiny mites known as Sarcoptes scabiei. If you’ve ever wondered how to identify scabies and distinguish it from other skin problems, you’re in the right place.
In this comprehensive guide, we will delve into the key signs and visual clues that can help you recognize this pesky condition. From the relentless itch to the telltale burrows, we’ll explore it all. So, let’s roll up our sleeves and uncover the secrets of identifying scabies.
Quick Navigation
- 1 Understanding Scabies
- 2 1. Unrelenting Itch
- 3 2. Pimple-like Rash
- 4 3. Burrows and Tracks
- 5 4. Secondary Infections
- 6 5. Spread in Close Contact
- 7 Who’s at Risk of Scabies?
- 8 Close Contacts
- 9 Children and Infants
- 10 Healthcare Workers
- 11 Elderly Individuals
- 12 Homeless Individuals
- 13 Sexual Partners
- 14 Immunocompromised Individuals
- 15 Travelers
- 16 Personal Hygiene and Living Conditions
- 17 When to Seek Medical Help for Scabies
- 18 Persistent Itching
- 19 Visible Skin Changes
- 20 Appearance of Secondary Infections
- 21 Outbreaks in Close Contacts
- 22 Suspected Scabies in High-Risk Populations
- 23 Failed Home Treatment
- 24 Infants and Young Children
- 25 Pregnancy
- 26 Immunocompromised Individuals
- 27 How to Identify Scabies: The Conclusion
Understanding Scabies
Before we delve into identifying scabies, it’s essential to grasp the basics of this condition. Scabies are caused by microscopic mites that burrow into the outer layer of your skin, laying eggs along their path. The infestation typically results in intense itching and a red, pimple-like rash. Let’s break down the key signs to watch out for:
1. Unrelenting Itch
One of the primary indicators of scabies is an unrelenting itch that worsens at night. This itchiness occurs due to the mites burrowing and laying eggs beneath the skin. While itching can affect any part of the body, it’s most common in areas where the mites are most active, such as between fingers, on the wrists, elbows, armpits, and genital area.
2. Pimple-like Rash
Scabies often present themselves with a pimple-like rash. This rash appears as small, red, and sometimes blistered bumps. It’s crucial to note that the rash can mimic other skin conditions like eczema or allergic reactions, which makes identifying scabies a bit challenging based on the rash alone.
3. Burrows and Tracks
A definitive sign of scabies is the presence of burrows, which are tiny, thread-like lines on the skin. These burrows are created by the mites tunneling beneath the skin’s surface. They can be challenging to spot, but you may find them on the webbing between fingers, on the wrists, and around the genital area.
4. Secondary Infections
Due to the constant scratching, scabies can lead to secondary bacterial infections. Look out for signs such as increased redness, warmth, swelling, or pus around the affected areas.
5. Spread in Close Contact
Scabies is highly contagious, and it spreads through close personal contact. If someone in your household or close social circle has scabies, there’s a good chance you might contract it too.
Who’s at Risk of Scabies?

Photo Credit: lybrate.com
Scabies is a highly contagious skin infestation caused by the Sarcoptes scabies mite. While anyone can contract scabies, certain groups are at a higher risk of infection due to their living conditions, behaviors, or personal characteristics.
Close Contacts
Individuals who have close and prolonged contact with an infected person are at a heightened risk. This includes family members, sexual partners, and caregivers. Scabies spreads through direct skin-to-skin contact, making people living in crowded households or institutions, such as nursing homes or prisons, more susceptible.
Children and Infants
Scabies can affect individuals of all ages, but it is particularly common among children and infants. Children often engage in close physical contact during play, and infants have more delicate skin, which can make them more vulnerable to infestations.
Healthcare Workers
Healthcare professionals, including nurses and doctors, may be at increased risk due to their frequent contact with patients. Hospitals and long-term care facilities can be hotspots for scabies transmission if proper infection control measures are not in place.
Elderly Individuals
Older adults, especially those residing in communal living environments like nursing homes, are at higher risk due to compromised immune systems, reduced mobility, and frequent interactions with caregivers or fellow residents.
Homeless Individuals
Homeless populations are more prone to scabies due to overcrowded shelters, limited access to sanitation facilities, and shared bedding or clothing. Poor living conditions can facilitate the spread of scabies in homeless communities.
Sexual Partners
Scabies can be transmitted through sexual contact, increasing the risk for individuals engaging in sexual activities with an infected partner. Safe sexual practices and awareness are essential for preventing transmission.
Immunocompromised Individuals
People with weakened immune systems, such as those with HIV/AIDS or undergoing chemotherapy, may be at greater risk of scabies infestation. Their compromised ability to fight off infections makes scabies harder to control and manage.
Travelers
Travelers visiting regions with higher scabies prevalence may be at risk of exposure. Tropical and subtropical areas often report higher rates of scabies cases.
Occupational Exposure: Certain occupations, such as those involving frequent contact with animals (veterinarians, farmers) or handling textiles (seamstresses), can increase the risk of scabies due to potential exposure to scabies-infested animals or fabrics.
Personal Hygiene and Living Conditions
Poor personal hygiene and living in unclean, crowded, or unsanitary environments can also elevate the risk of scabies infestation.
When to Seek Medical Help for Scabies

Scabies, caused by the Sarcoptes scabies mite, is a highly contagious skin condition that can be uncomfortable and persistent if left untreated. It is essential to recognize when to seek medical assistance for scabies to prevent complications and ensure effective treatment.
Persistent Itching
The hallmark symptom of scabies is intense itching, particularly at night. If itching persists or worsens after a few days, medical attention is necessary. Prolonged itching can lead to skin infections due to scratching.
Visible Skin Changes
If you notice new rashes, pimple-like bumps, or small, raised, thread-like burrows on your skin, especially in the webbed areas between fingers, toes, wrists, elbows, armpits, or genitalia, it’s a clear sign of scabies. Seeking prompt medical evaluation is crucial for proper diagnosis.
Appearance of Secondary Infections
Scratching the scabies rash can break the skin, increasing the risk of bacterial infections. If you notice signs of infection like increased redness, warmth, swelling, pus, or fever, consult a healthcare professional immediately.
Outbreaks in Close Contacts
If someone you’ve had close contact with is diagnosed with scabies, it’s advisable to seek medical advice even if you haven’t developed symptoms yet. Early intervention can prevent the infestation from spreading further within your household or community.
Suspected Scabies in High-Risk Populations
In settings where scabies can have severe consequences, such as nursing homes, schools, or childcare centers, individuals with suspected scabies should seek medical evaluation promptly. Timely diagnosis and treatment can help prevent outbreaks in such environments.
Failed Home Treatment
Over-the-counter treatments for scabies may not always be effective. If self-treatment does not alleviate symptoms or if they recur after initial relief, consult a healthcare provider for prescription medications.
Infants and Young Children
Scabies can present differently in infants and young children, often with more extensive rashes and itching. If your child exhibits signs of scabies, consult a pediatrician for appropriate diagnosis and treatment.
Pregnancy
Pregnant or breastfeeding women with scabies should seek medical advice before using any medications, as some treatments may not be suitable during pregnancy or while nursing.
Immunocompromised Individuals
People with weakened immune systems, such as those with HIV/AIDS or receiving immunosuppressive therapies, may experience atypical or severe scabies infestations. Medical guidance is crucial for their care.
How to Identify Scabies: The Conclusion
In conclusion, identifying scabies requires a keen eye for the specific signs and visual clues associated with this condition. These include the relentless itch, pimple-like rash, burrows and tracks, and the possibility of secondary infections. If you suspect you have scabies or have been in close contact with someone who does, it’s crucial to seek medical attention promptly. A healthcare professional can diagnose scabies and recommend appropriate treatment options, typically involving topical creams or oral medications.
In this blog, we’ve explored “How to Identify Scabies” and its key signs and visual clues. Identifying scabies is the first step towards effective treatment and preventing their spread. If you suspect you have scabies or have been in close contact with someone who does, seek medical attention promptly. Remember, early intervention is essential in managing this condition.
References:
- Strong, M., & Johnstone, P. (2007). Interventions for treating scabies. Cochrane Database of Systematic Reviews, (3).
- World Health Organization. (2018). Scabies and Other Ectoparasites. Retrieved from https://www.who.int/neglected_diseases/diseases/scabies/en/
- Hay, R. J., Steer, A. C., Chosidow, O., & Currie, B. J. (2012). Scabies: a suitable case for a global control initiative. Current Opinion in Infectious Diseases, 25(2), 131-139.
